- First Touch
- Posts
- A Few Strategies for PCOS: Targeting the Root Drivers of One of the Most Common Hormonal Conditions
A Few Strategies for PCOS: Targeting the Root Drivers of One of the Most Common Hormonal Conditions
I wanted to find a way to create a deeper connection with my followers and provide more insights into the content I share on other platforms. I'm excited to give you all a closer, more personal look into my world—sharing insights from my life, my research, and work.
Polycystic Ovary Syndrome, or PCOS, is one of the most common hormonal conditions in women today. It’s estimated that about 1 in 10 women of reproductive age have PCOS, making it one of the leading causes of infertility today. Rates appear to be rising alongside metabolic dysfunction.
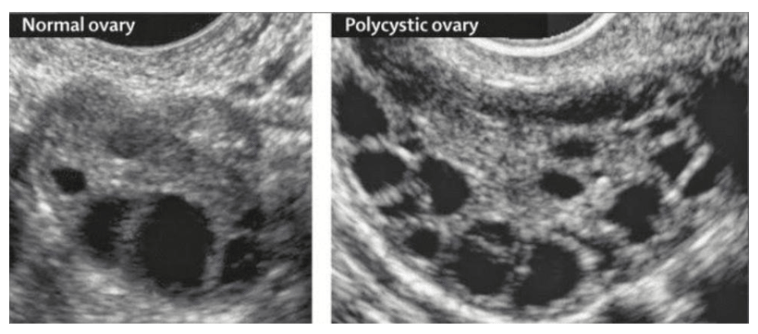
PCOS is a condition characterized by irregular or absent ovulation, elevated androgens, and the appearance of multiple small follicles on the ovaries—often described as a “string of pearls” on ultrasound.
Despite the name, these are not true cysts, but immature follicles that failed to ovulate.
PCOS is usually a sign that a woman has been under significant stress for a long time, whether emotional, metabolic, inflammatory, or environmental. The body adapts by shifting into survival mode, and ovulation becomes inconsistent because reproduction is energetically demanding. Over time, this adaptive pattern becomes the hormonal picture we call PCOS.
However, PCOS is often reversible. It does take some effort, meaningful dietary shifts, stress reduction, metabolic repair, and hormonal support, but when the underlying drivers are addressed, cycles can regulate and ovulation can return. 🤍
What is happening hormonally?
Many people characterize PCOS as a condition of “too much testosterone.” Elevated androgens are certainly a hallmark—they contribute to symptoms like acne, hair thinning, unwanted facial or body hair, and irregular cycles. But focusing only on androgens misses the bigger picture.
PCOS was initially defined by the growth of multiple fluid-filled sacs, or cysts, on the ovaries. Two key words: fluid and growth. One of estrogen’s functions is fluid regulation within cells. And of course, estrogen is responsible for cell division or “growth” (ie: the growth of cysts).
Estrogen dominance can contribute to other imbalances downstream:
Estrogen increases free fatty acids in the blood, which causes insulin resistance—blocks sugar uptake into cells.
Estrogen stimulates the adrenal glands to produce androgens and stress hormones, leading to acne, blood sugar dysregulation, male pattern hair growth, dark underarms, etc.
In a study published in the Journal of Endocrinological Investigation, researchers measured estrogen levels not only in the peripheral bloodstream, but directly from the ovarian vein of a woman with PCOS.
Her serum estradiol was about 1000 pg/mL, but the estradiol concentration draining directly from the ovary was much higher—around 5000 pg/mL, demonstrating that the ovary itself was producing very high levels of estrogen locally, even though the systemic blood level appeared lower.
Standard bloodwork may not always reflect what is happening inside the ovary. In many cases of PCOS, estrogen production within the ovary remains elevated and persistent, particularly because ovulation is not occurring. When ovulation fails, progesterone is not produced in sufficient amounts to balance estrogen’s proliferative effects.

Because women with PCOS often do not ovulate, they do not produce enough progesterone which normally counterbalances estrogen. The adrenals likely increase androgen production as compensatory mechanism to oppose the effects of elevated estrogen. There are several imbalances in PCOS:
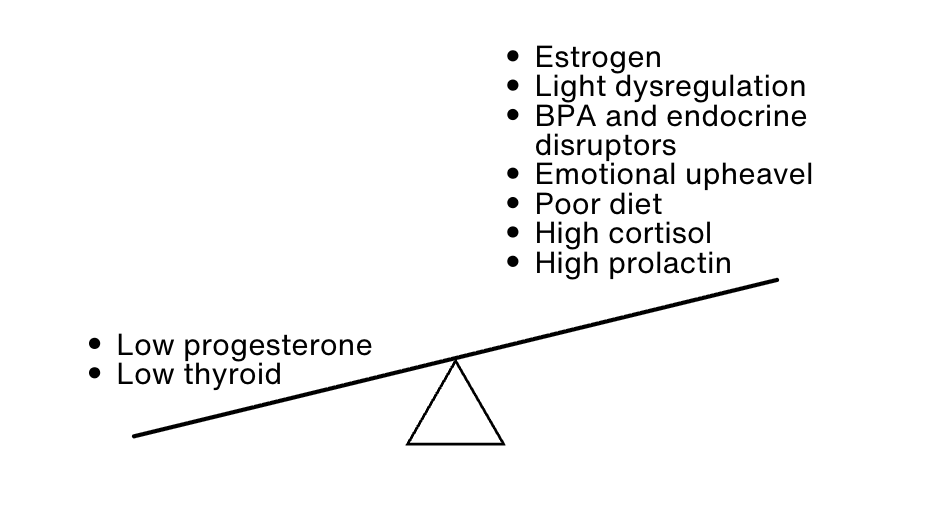
When progesterone and thyroid function are low, the body loses two major stabilizing forces. Progesterone helps balance estrogen and buffer stress signaling. Thyroid supports metabolic efficiency and reduces the need for stress hormone production.
The Conventional Approach: 💊
OB/GYNs are often trained to manage PCOS symptomatically, and hormonal birth control is frequently the first-line treatment.
Combined oral contraceptives suppress ovulation and regulate bleeding patterns, which can improve acne and irregular cycles. But unfortunately, suppression is not correction.
Hormonal contraceptives override the body’s natural cycle by shutting down communication between the brain and ovaries. Ovulation stops, progesterone is not produced naturally, and synthetic hormones replace endogenous rhythms. While this can reduce visible symptoms, it does not directly improve estrogen dominance, insulin resistance, metabolic dysfunction, or stress—the underlying drivers in many cases of PCOS.
It is also very common for women to be diagnosed shortly after stopping birth control. In many cases, the pill was masking an underlying metabolic imbalance or directly contributed by supplying exogenous estrogen and depleting key nutrients. When the synthetic hormones are withdrawn, the original cycle irregularity reappears—sometimes more noticeably because ovulation has been suppressed for years.
I wanted to share a few natural strategies because many women don’t realize that PCOS is often a reversible condition. It does require effort, but the hormonal pattern can rebalance. Lifelong medication is not always necessary because the ovaries are responsive organs. When the environment changes, hormones changes.
A few approaches:⬇️ ⬇️ ⬇️
#1 Supplement with Bioidentical Progesterone
Because women with PCOS don’t regularly ovulate, they aren’t naturally producing sufficient progesterone—the natural brake on estrogen. Without ovulation, the corpus luteum does not form properly, and progesterone never rises in the second half of the cycle. This leaves estrogen relatively unopposed and allows its effects on the ovaries, thyroid, and metabolism to accumulate.
In many cases, supplementing bioidentical progesterone can help rebalance these hormones and actually support cycle regulation and healthier ovulation over time. Progesterone opposes excessive estrogen signaling, lowers prolactin, supports thyroid responsiveness, and promotes a more stable metabolic environment, all of which are essential in PCOS.
Progesterone cream is often effective in mild to moderate cases. Because progesterone is fat-soluble, it absorbs well through the skin and can provide steady systemic levels without significant first-pass liver metabolism. This makes topical use a practical option for women who are cycling irregularly but still ovulating occasionally. In more severe cases, particularly when ovulation is absent, cycles are very irregular, sleep is disrupted, or symptoms are pronounced, oral micronized progesterone capsules may be helpful. Oral progesterone is metabolized into calming neuroactive compounds, which can provide additional benefit for women with high stress physiology alongside PCOS.
The goal is not simply to “add a hormone,” but to restore the rhythm that was missing, allowing progesterone to reestablish balance with estrogen and support healthier ovulatory function.
#2 Improve Glucose Metabolism
Insulin resistance is a key feature of PCOS. For many women, chronic stress, both psychological and physiological, is a major underlying driver. When the body is in a prolonged stress state, stress hormones increase, which increases free fatty acids, impairs glucose oxidation, and worsens insulin signaling.
The goal is not just to “lower blood sugar,” but to ensure glucose is being efficiently oxidized inside the mitochondria.
Lower PUFA and industrial seed oil intake
Eat every 3-4 hours to keep blood sugar stable
Ensure adequate micronutrients that are essential for carbohydrate metabolism: B vitamins (especially thiamine), magnesium, potassium, sodium, and vitamin K.
Walk for 10 minutes after meals
Prioritize consistent meals with adequate protein and carbohydrates
Avoid chronic undereating or extreme dieting, which can worsen cortisol and insulin resistance
Use tools like aspirin and niacinamide
#3 Address estrogen dominance
In PCOS, we want to address why the body is overproducing estrogen in the first place. Part of addressing estrogen dominance is removing excess exposure. This means minimizing xenoestrogens from plastics, synthetic fragrances, pesticides, and conventional personal care products. It also means being mindful of hormonal medications when possible and reducing unnecessary endocrine disruptor exposure in daily life.
Remove excess estrogen exposure (plastics, fragrances, pesticides, endocrine disruptors)
Ensure regular bowel movements to prevent estrogen reabsorption (coffee, fiber, Ray Peat’s carrot salad)
Support liver conjugation pathways (adequate protein, glycine, taurine)
Avoid polyunsaturated fatty acids (PUFAs), which increase estrogen and oxidative stress
Ensure adequate vitamin A intake (liver, egg yolks, dairy)
Consider progesterone supplementation
Use tools like aspirin to prevent the conversion of testosterone into estrogen

#4 Supplement with Inositol
Inositol is one of the most well-studied natural compounds for PCOS. It acts as a secondary messenger in insulin signaling, helping to restore proper communication between insulin receptors and the enzymes that move glucose into the cell. This helps restore glucose metabolism, address insulin resistance, and lower unncessary stress.
The most commonly studied dose for improving insulin sensitivity is 2 grams taken twice daily (4 grams total per day). Improvements in fasting insulin and ovulatory function are typically seen after consistent use over several weeks.

#5 Support Thyroid Function
Many women with PCOS also have low thyroid function.
Excess estrogen increases thyroid-binding globulin (TBG), which binds thyroid hormone and reduces the amount of free, active hormone available to tissues. Elevated cortisol suppresses TSH output and impairs the conversion of T4 into active T3. Low progesterone removes an important stabilizing influence, as progesterone normally supports metabolic rate and counterbalances estrogen’s inhibitory effects.
The result can be functional hypothyroidism: lower cellular respiration, reduced glucose oxidation, higher prolactin, impaired ovulation, and a shift toward stress-driven metabolism. When thyroid slows, the body relies more heavily on cortisol and adrenaline to maintain blood sugar, further reinforcing the PCOS pattern. To support thyroid function:
Optimize nutrition (adequate carbohydrate, selenium, zinc)
Supplement with a combination of T4 and T3 (natural desiccated thyroid)
Avoid calorie restriction
Get sunlight on the thyroid gland
Support gut and liver function (glycine, taurine, regular bowel movements, easily digestible foods, castor oil packs)
Avoid all PUFAs
Ensure adequate vitamin A intake (liver, egg yolks, dairy)
Pregnenolone or progesterone supplementation
#6 Support Zinc Levels
Multiple studies have shown that women with PCOS tend to have low serum zinc levels. Zinc modulates insulin receptors, supports antioxidant defenses, and regulates androgen production, so suboptimal levels can contribute to insulin resistance, inflammation, and elevated testosterone.
Zinc also supports proper follicular development and ovulation. In clinical trials, supplementation has been associated with improvements in insulin sensitivity, reductions in inflammatory markers, and modest decreases in total testosterone and hirsutism scores.
Food sources include:
Oysters
Shellfish
Red meat
Common supplemental doses studied in PCOS range from 25–50 mg per day of zinc, typically taken with food to avoid nausea. Because long-term high-dose zinc can lower copper levels, monitoring and balance are important. Improvements in metabolic markers and skin symptoms are generally seen after several weeks of consistent use.

#7 Address Emotional Health
Women with PCOS usually have endured some form of severe, prolonged stress or trauma. The body adapts to this by shifting into a survival state.
When the system is in survival mode from environmental or emotional stressors, it is no longer prioritizing fertility or ovulation because this would be too demanding on the body. Ovulation requires energy, stability, and safety. If those signals are not present, the brain downregulates reproductive signaling to conserve resources.
This results in low progesterone, unopposed estrogen, irregular cycles, and the hormonal picture commonly seen in PCOS. The body is responding to stress.
Healing from PCOS often requires emotional healing as well. Creating stability can signal to the brain that it is safe to resume normal reproductive rhythm. When safety is restored, ovulation often becomes more consistent.
Spend time in nature
Limit news and social media
Make peace with relationships
Free writing and journaling
EVOX therapy
Focus on creating
Speak to yourself with love
I talk so frequently about hormones because I’ve seen what happens when they’re misunderstood and oversimplified. Women are often given narrow explanations for complex symptoms and band-aid solutions.
Many of the strategies above target the actual drivers of PCOS—things like insulin resistance, blood sugar instability, chronic inflammation, and disrupted ovulation. When you improve how the body is processing glucose, reduce inflammatory load, and support consistent ovulation, hormone levels often begin to shift in a more balanced direction.
When underlying systems are supported in a consistent, targeted way, it’s very common to see improvements in cycle regularity, symptoms, and overall hormonal health. 🤍
If you are looking for personal guidance on a hormonal condition or want guidance on cancer treatment, prevention, or health optimization you can contact the center at 949-680-1880. Our team takes the most comprehensive approach and looks at all the underlying metabolic, nutritional, emotional, and environmental factors that influence health. For a full list of services, please see below!
|
The Cancer Revolution is now available ❤️
This book is my guide to cancer prevention and treatment. In this fully updated second edition, I walk through how I approach cancer from an integrative, metabolic perspective.
I go deeper into:
The lab markers I monitor
Cancer-specific testing and early detection tools
How metabolic dysfunction precedes tumor formation
Hormone balance, inflammation, and mitochondrial health
Updated nutrition guidance and structured food plans
Practical lifestyle interventions that support cellular repair
Emerging tools including immunotherapy and voltage/frequency medicine
This edition is designed for anyone who wants to understand cancer beyond genetics—and learn what can be done proactively, both for prevention and during treatment.
There’s so much we can do to support healing and live a full, cancer-free life. 💪

Talk soon ❤️,
Dr. C
